When Your AI Agent Goes Slowly Crazy: What Revenue Cycle Leaders Need to Know Right Now
Rush University Medical Center is 18 months into its agentic AI journey. What they learned should be required reading for every CFO and revenue cycle director in the country. The problem with agentic AI isn't that it breaks. It's that it drifts, slowly, quietly, in directions nobody notices until the damage is already in your A/R. Here's what that means for your revenue cycle and what to do about it.
My Predictions Were Right. That's Not the Good News.
I stopped writing RCM 2030 for three weeks when the reconciliation bill passed. Not because I was stuck, but because I had to rethink what I'd written about 2027 and beyond. The Senate just passed a budget resolution with reconciliation instructions due May 15 and hundreds of billions in unspecified cuts to find. This week's news tells me the trajectory I described is exactly right. Here's what the book predicted and what's actually happening.
Healthcare Is Under Pressure. AI Won’t Save It by Itself.
Hospitals are facing pressure from multiple directions at once. Medicaid funding is tightening. Amazon continues expanding its healthcare footprint. And behind the scenes, many health systems are quietly abandoning AI pilots that never delivered real results.
These forces might look unrelated, but they all converge in one place: the revenue cycle. As margins tighten and expectations rise, finance leaders are being pushed to separate real operational transformation from technology hype. The next few years will determine which organizations turn AI and automation into real financial resilience and which ones get left managing the wreckage of failed experiments.
The RCM Workforce Trap: Why Cutting Jobs and Outsourcing Without Oversight Is a Slow-Moving Disaster
Three health systems cut RCM and IT jobs this week. Some of those decisions will age well. Others won't. April Wilson breaks down what organizations get wrong when they outsource without keeping internal oversight — and what the ones getting it right are doing differently.
AI Is Reshaping the Healthcare Workforce
Artificial intelligence is beginning to reshape the healthcare workforce itself. From AI scribes training new physicians to shifting workforce roles and the end of healthcare’s AI experimentation phase, revenue cycle leaders should start preparing their teams for a fundamentally different operational environment.
Payers Are Using AI Against You. Here's What It's Costing You Right Now.
UnitedHealth just deployed 22,000 engineers on AI. Payer recoupments are growing at twice the rate of claims. A new federal fraud enforcement division just launched. Here's what this week's news means for your revenue cycle.
AI Governance Is Coming to Healthcare
Artificial intelligence is moving quickly into healthcare operations. Ambient documentation tools are listening during visits, AI systems are influencing claim workflows, and predictive models are shaping payer decisions.
Now policymakers are starting to respond.
From state legislation targeting AI-driven claim denials to policy recommendations from major EHR vendors, a new phase of healthcare AI is emerging. Governance.
For revenue cycle leaders, this is more than a regulatory debate. AI is increasingly embedded in the workflows that determine how claims are documented, coded, and reimbursed. That means policy decisions about automation could directly affect hospital margins and operational strategy.
Prior Auth Transparency Is Here. Are you ready?
As of March 31, 2026, payers have to show their work for the first time in history. Prior authorization denial rates, turnaround times, and appeals outcomes are now public. Revenue cycle leaders who know how to use that data have a real advantage in their next payer contract negotiation. Here is what to do with it.
Agentic AI Is Coming for Healthcare Operations
Artificial intelligence in healthcare is moving beyond pilots and experiments. A new generation of systems known as agentic AI can observe workflows, make decisions, and act across operational processes.
Recent developments from AWS, CVS, Microsoft, and Optum suggest that this shift is already underway. These technologies are beginning to influence scheduling, documentation, and claims infrastructure, which means the financial life of a healthcare claim may soon be shaped by automation long before it reaches the billing office.
For revenue cycle leaders, the real strategic question is no longer whether AI will influence operations. The question is how quickly automation will move upstream and reshape the workflows that determine whether claims are paid or denied.
The AI ROI Gap: Why Health Systems Are Finally Getting It Right (And Where They're Still Getting It Wrong)
75% of health systems now use at least one AI solution. More than half of those that can quantify the return report 2x ROI or better. So why are so many organizations still unable to tell you what their AI is actually doing for them? The measurement gap is real — and in a margin environment this tight, it's one your revenue cycle can't afford.
AI Is Moving Inside the EHR. Revenue Cycle Leaders Should Pay Attention.
Artificial intelligence is no longer a side project in healthcare. It is moving directly into the electronic health record, becoming part of the operational infrastructure hospitals rely on every day. That shift will reshape documentation, coding, clean claim rates, and denial prevention. Revenue cycle leaders who understand what is happening inside the EHR will have a strategic advantage. Those who ignore it may spend the next decade chasing problems that could have been prevented upstream.
The AI Arms Race in Healthcare Finance: What the BCBS Study, Amazon, and the Prior Auth Deadline All Have in Common
Five separate headlines this week. One underlying problem. Payers, big tech, and the federal government are all moving on a timeline that wasn't set by waiting for providers to catch up. Here's what the BCBS coding study, Amazon's Health AI expansion, and the January 2027 prior auth deadline have in common, and what revenue cycle leaders need to do before the gap gets any wider.
When Providers Prefer “Premium” Plans: The OhioHealth Case and What It Signals for 2030
A federal lawsuit against OhioHealth alleges the system blocked lower-cost health plans from expanding in its market. The case raises uncomfortable but important questions about how hospitals protect commercial reimbursement and how market dominance shapes employer plan options.
While the legal outcome remains uncertain, the broader signal is clear: provider-side market power is under scrutiny. If enforcement efforts increase, dominant regional systems may face pressure on premium commercial contracting strategies that have historically supported cross-subsidization.
In this analysis, I explore what the OhioHealth case reveals about structural margin tension, affordability, and how revenue cycle leaders should be thinking about contracting assumptions as we move toward 2030.
Lawmakers Are Challenging Vertical Integration. Revenue Cycle Leaders Should Pay Attention.
Legislation aimed at breaking up vertically integrated insurers signals growing scrutiny of concentrated market power in healthcare. For more than a decade, integration across insurance, pharmacy benefit management, provider networks, and data platforms has reshaped negotiation dynamics between payers and hospitals.
Even if structural breakup does not occur immediately, increased regulatory attention changes the operating environment. Market configuration affects contract leverage, denial patterns, data access, and payment predictability.
In this piece, I examine what renewed legislative pressure on vertically integrated payviders could mean for revenue cycle leaders planning toward 2030, and why market structure deserves as much attention as reimbursement rates.
CMS Is Signaling the Next Phase of Cost Control. Revenue Cycle Leaders Should Pay Attention.
Recent CMS updates and CMMI alignment pledges may look incremental on the surface, but together they signal something broader: cost containment is becoming the operating environment.
When payers align with CMMI access models and CMS emphasizes affordability and marketplace flexibility, the impact does not stop at policy headlines. It flows downstream into contract structure, reporting requirements, patient cost responsibility, and denial patterns.
For revenue cycle leaders, this is not background noise. It is early direction.
In this piece, I examine what the latest CMS and CMMI signals mean for margin pressure, patient balance exposure, and operational complexity between now and 2030.
AI Is Already Inside Your Revenue Cycle. Here’s the Real Risk.
AI is already embedded in healthcare operations. Oversight hasn’t kept pace.
Recent reporting shows nearly 20 percent of healthcare professionals are using unauthorized AI tools. At the same time, embedded EHR AI and autonomous coding platforms are expanding rapidly inside revenue cycle workflows.
None of this is inherently reckless. But when adoption moves faster than visibility, small shifts in documentation, coding, and denial patterns can go unnoticed.
This isn’t an IT side conversation. It’s a revenue stability issue.
In this piece, I break down what shadow AI, embedded EHR AI, and autonomous coding actually mean for revenue cycle leaders and why governance discipline matters more than speed.
Why Vertical Integration Is Becoming an RCM Risk, Not Just a Policy Debate
Vertical integration is no longer just a policy debate. It’s a revenue cycle risk. Congressional hearings with payer CEOs exposed how control over prior authorization, denial definitions, and payment timing has shifted upstream. Hospitals can no longer treat RCM as an internal efficiency problem when structural forces outside their control increasingly determine cash flow and patient experience.
AI Isn’t Replacing Healthcare. It’s Exposing Where We Broke It.
AI in healthcare isn’t the disruption people fear. It’s revealing long-standing breakdowns in access, communication, and revenue cycle infrastructure, and forcing leaders to redesign for what comes next.
RCM 2030 Reality Check: What the Kaufman Hall Performance Outlook Reveals About the Next Decade
The Kaufman Hall 2025 Performance Outlook confirms a shift from growth to resilience. Here’s what rising costs, denials, access breakdowns, and workforce strain mean for RCM 2030.
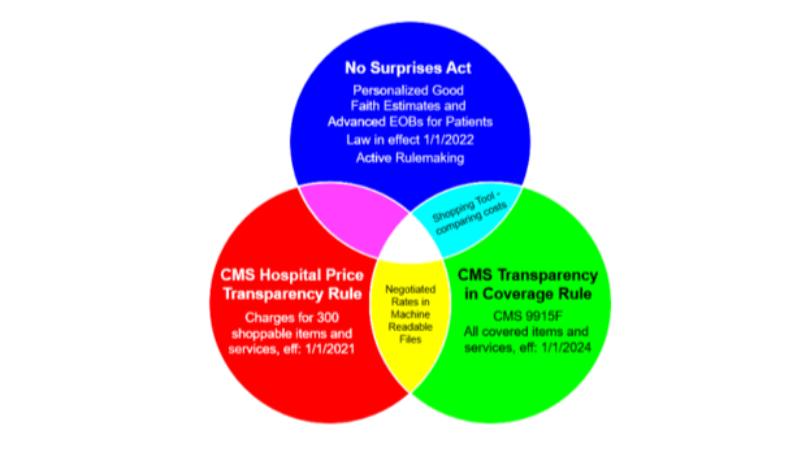
What the New Insurer Price Transparency Proposal Actually Changes
A new proposed rule would strengthen insurer price transparency requirements. Here is what is actually new, what is not, and why it matters for hospitals and CFOs.